Falls represent one of the most serious threats to older adults living at home, often leading to injuries, loss of independence, and even death. As the leading cause of fatal and non-fatal injuries for those aged 65 and older, falls affect one in four adults in this group annually, with many incidents going unreported due to fears of losing autonomy. 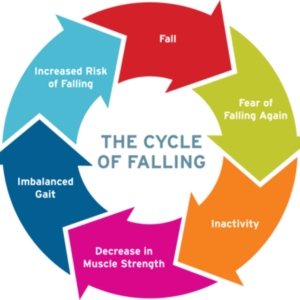 The consequences extend beyond physical harm, triggering a vicious cycle of fear, reduced activity, muscle weakness, poor balance, and heightened future risk. In home care, caregivers play a vital role in spotting risks early, implementing practical changes, and knowing when to escalate concerns. Proactive prevention preserves safety and quality of life.
The consequences extend beyond physical harm, triggering a vicious cycle of fear, reduced activity, muscle weakness, poor balance, and heightened future risk. In home care, caregivers play a vital role in spotting risks early, implementing practical changes, and knowing when to escalate concerns. Proactive prevention preserves safety and quality of life.
1. Three Indicators of Increased Fall Risk
Multiple factors compound fall risk, with each additional one amplifying danger. Key indicators include:
- – History of previous falls. The strongest predictor; a prior fall significantly raises the likelihood of another.
- – Lower body weakness or balance/gait difficulties. Signs include struggling to rise from a chair without using arms, “furniture surfing” (holding onto furniture while walking), or losing balance during simple tasks like putting on a shirt.
- – Vision problems. Issues such as poor night vision, reduced contrast sensitivity, glaucoma, cataracts, or not wearing needed glasses impair hazard detection.
Other notable risks encompass vitamin D deficiency, polypharmacy (especially sedating medications like tranquilizers or antidepressants), foot pain or improper footwear (e.g., slippery slippers), and postural hypotension (dizziness upon standing).
2. Key Questions Regarding Fall Risk
Simple, evidence-based questions quickly flag elevated risk, as recommended by CDC’s STEADI initiative. A “yes” to any signals increased concern:
- – Have you fallen in the past year?
- – Do you feel unsteady when walking or standing?
- – Do you worry about falling?
These questions, drawn from validated tools, help identify at-risk individuals even without a formal screen. Positive responses warrant further attention, such as discussing modifiable factors or environmental adjustments.
3. Environmental Modifications to Reduce Fall Risk
Home hazards cause most falls, particularly in bathrooms, but targeted changes dramatically improve safety. Two high-impact modifications:
- – Remove tripping hazards and improve lighting — Eliminate loose throw rugs (or secure with non-slip backing), clear clutter and cords from walkways, and install motion-activated night lights or bright, glare-free bulbs in hallways, bedrooms, and bathrooms to prevent nighttime stumbles.
- – Install supportive features in high-risk areas — Add grab bars near toilets and in showers/tubs (consider stylish or suction-cup options if permanent installation concerns arise), and use non-slip mats, shower chairs, or transfer benches to enhance stability during bathing.
Additional helpful steps include securing handrails on stairs, rearranging frequently used items to avoid reaching or climbing, and encouraging supportive footwear over slippers.

4. When is a Referral Is Appropriate?
Referrals ensure timely intervention for modifiable risks. In home care, escalate to a supervisor, physician, or specialist when:
- – The client reports a recent fall, shows clear signs of unsteadiness, or answers “yes” to key risk questions — prompting evaluation for physical therapy (to build strength, balance, and safe falling techniques), medication review (to address polypharmacy or side effects), vision/foot exams, or home safety assessments.
- – A pattern emerges, such as repeated near-falls, off-shift incidents, or failure to use prescribed assistive devices (e.g., walker) — this may justify added shifts, gait belt use, hands-on assistance requirements, or discussions about increased support.
Any fall, even minor or unreported previously, requires documentation via incident report to track trends and inform care adjustments.
Fall prevention empowers older adults to stay safely in their homes. By recognizing indicators, asking targeted questions, making straightforward environmental tweaks, and referring promptly, caregivers interrupt the cycle of falls and support lasting independence. Vigilance today prevents crises tomorrow—small actions yield profound protection.
STACEY WELFEL
Director of Training & Compliance
Mrs. Welfel serves as Director of Training and Compliance. She has more than 15 years of clinical experience as a neurological physical therapist, most of which was spent working with catastrophic rehab clients at TIRR Memorial Hermann Hospital. She currently works as a physical therapist and clinical coordinator for Rehab Without Walls, a unique rehabilitation concept providing patients with neurological injuries the functional skills necessary to return to their home and community.

